Health Information
Jaundice Baby…Home Phototherapy…Safe & Easy
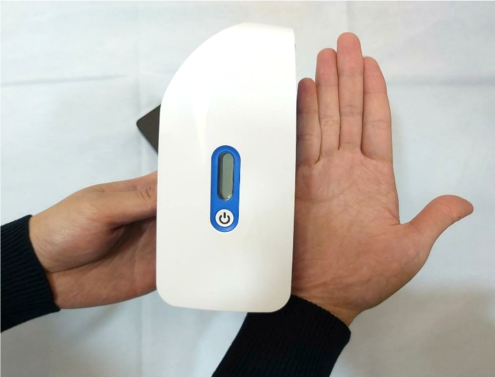
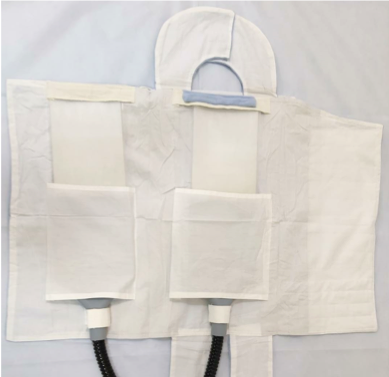
What is it?
Japanese encephalitis (JE) is a vector-borne zoonotic viral disease. JE virus (JEV) is the leading cause of viral encephalitis in Asia. JE occurs in nearly all Asian countries, whether temperate, subtropical, or tropical, and has intruded into new areas through importation of infected vectors. Currently, an estimated 3 billion people live in the 24 countries, mainly in the WHO South-East Asia and Western Pacific Regions, considered at risk of JE.1
In temperate locations, the period of transmission of JEV typically starts in April or May, and lasts until September or October. In tropical and subtropical areas, transmission exhibits less seasonal variation, or intensifies with the rainy season.20
As JE surveillance is not well established in many countries, and laboratory confirmation is challenging, the true extent and prevalence of the virus and burden of disease are not well understood. It is estimated that 67 900 clinical cases of JE occur annually despite widespread availability of vaccine, with approximately 13 600 to 20 400 deaths, and an overall incidence rate of 1.8/100 000 in the 24 countries with JE risk.1
Mode of transmission
JEV is transmitted through a zoonotic cycle between mosquitoes, pigs and water birds. Humans get accidentally infected when bitten by an infected mosquito and are a dead end host. Humans do not participate in the spread of JE because of low level and short-lived viremia.2

Signs and symptoms3
Symptoms usually start at around 4-14 days after being infected. Mild infections may occur without apparent symptoms other than fever with headache. More severe infection is marked by quick onset of headache, high fever, neck stiffness, impaired mental state, coma, tremors, occasional convulsions (especially in children) and paralysis.
Treatment and complications3
There is no specific treatment for this disease. Supportive therapy is indicated. Death rates may range from 5% to 35%. Patients who survive may have neurological consequences.
Prevention
WHO recommendations: JE vaccination should be integrated into national immunization schedules in all areas where JE is recognized as a public health priority. Even if the number of JE-confirmed cases is low, vaccination should be considered where there is a suitable environment for JEV transmission, i.e. presence of animal reservoirs, ecological conditions supportive of virus transmission, and proximity to other countries or regions with known JEV transmission.1
Besides, to prevent contracting the disease, one should take general measures to prevent mosquito bites, apply effective insect repellents (containing DEET) to exposed parts of the body and avoid going to rural areas from dusk till dawn when the mosquitoes spreading this virus are most active.22
General Measures on Preventing Mosquito-borne Diseases:3
- Wear loose, light-coloured, long-sleeved tops and trousers, and apply effective insect repellents containing DEET to exposed parts of the body & clothing.
- Use mosquito screens or bed nets when the room is not air-conditioned.
- Apply household pesticide to kill adult mosquito with a dosage according to the label instructions. Do not spray the pesticides directly against functioning electrical appliances or flame to avoid explosion.
- Place mosquito coil or electric mosquito mat / liquid near possible entrance, such as window, to prevent mosquito bites.
- Prevent the accumulation of stagnant water
- Put all used cans and bottles into covered dustbins.
- Change water for plants at least once a week, leaving no water in the saucers underneath flower pots.
- Cover tightly all water containers, wells and water storage tanks.
- Ensure air-conditioner drip trays are free of stagnant water.
- Keep all drains free from blockage.
- Top up all defective ground surfaces to prevent the accumulation of stagnant water.
Reference:
- World Health Organization. Japanese encephalitis: WHO position paper. 2015.
- Misra UK, Kalita J. Overview: Japanese encephalitis. Prog Neurobiol 2010; 91: 108–120.
- Centre for Health Protection. Communicable diseases – Japanese Encephalitis. 2016. doi:http://www.chp.gov.hk/en/content/9/24/28.html.
What is it?
In most countries, meningococcus is recognized as a leading cause of meningitis and fulminant septicaemia. It is classified into 12 serogroups based on the structure of the polysaccharide capsule. The majority of invasive meningococcal infections are caused by organisms expressing one of the serogroup A, B, C, X, W135 or Y capsular polysaccharides.
Neisseria species, which usually reside asymptomatically in the human nasopharynx, are easily transmitted to close contacts by respiratory droplets. Nasopharyngeal carriage of potentially pathogenic N. meningitidis has been reported in 4%–35% of healthy adults.1
Clinical features
Symptoms of invasive meningococcal disease (IMD) usually occur 1–4 days after infection. Signs and symptoms of IMD in infants and young children include fever, poor feeding, irritability, lethargy, nausea, vomiting, diarrhoea, photophobia and convulsions. The characteristic feature of meningococcal septicaemia is a hemorrhagic (petechial or purpuric) rash that does not blanch under pressure. Signs of meningitis in older children and adults include neck rigidity, photophobia and altered mental status, whereas in infants non-specific presentation with fever, poor feeding and lethargy is common. Besides meningitis and septicaemia, meningococci occasionally cause arthritis, myocarditis, pericarditis and endophthalmitis.
Most untreated cases of meningococcal meningitis and or septicaemia are fatal. Even with appropriate care up to 10% of patients die, typically within 24–48 hours of the onset of symptoms. Approximately 10% to 20% of survivors of meningococcal meningitis are left with permanent sequelae such as mental retardation, deafness, epilepsy, or other neurological disorders.
Mode of transmission
The disease is mainly transmitted by direct contact through respiratory secretions from infected persons.
Management
Meningococcal infection is a serious illness. Patients should be treated promptly with antibiotics. Close contacts would need to be placed under medical surveillance for early signs of disease and may be given preventive medications.
Prevention
Maintain good personal and environmental hygiene.
WHO recommendations: In countries where the disease occurs less frequently, meningococcal vaccination is recommended for defined risk groups, such as children and young adults residing in closed communities, e.g. boarding schools. Travellers or overseas students to high-endemic areas should be vaccinated against the prevalent serogroup(s). In addition, meningococcal vaccination should be offered to all individuals suffering from immunodeficiency, including asplenia, terminal complement deficiencies, or advanced HIV infection. Meningococcal vaccines against A, C, W, Y serogroup and vaccine against B serogroup are now registered in Hong Kong.
Hepatitis A is a viral hepatitis caused by the Hepatitis A virus. It is transmitted via intake of contaminated food (e.g. undercooked shellfish) or drinking water. Symptoms include diarrhoea, vomiting, fever and jaundice. Hepatitis A infection does not cause chronic liver disease and is rarely fatal, but it causes debilitating symptoms and fulminant hepatitis, which is associated with high fatality rates.
There is no specific treatment for hepatitis A. Therapy is aimed at maintaining comfort and adequate nutritional and fluid balance. Immunization is effective in preventing Hepatitis A infection and is recommended to residents and travelers to endemic regions (e.g. Mainland China, south-east Asia).
Rotavirus damages the cells on the hair-like projections of the small intestine, reducing their ability of absorption, causing diarrhoea. It is the leading cause of severe, dehydrating diarrhoea in children under the age of 5 years globally. Features of the disease include fever, vomiting and watery diarrhoea. The disease lasts for 3-7 days and young children are at particular risk of dehydration.
Rotavirus is highly contagious. It is transmitted via fecal-oral route, through consumption of contaminated food or water, or by contact with contaminated surface. To date there is no drug available as specific treatment to Rotavirus. Supportive treatment, such as intravenous fluids administration to prevent dehydration and antipyretics, are mainstay of treatment. Disease can be prevented by oral vaccines available to infants.
Vaccines are available in 2-dose or 3-dose from. Infants can be vaccinated from 6 weeks of age. Depend on the brand chosen, the schedule need to be completed by 24 weeks or 32 weeks.
Haemophilus influenzae is a bacterium that causes severe invasive infections such as pneumonia, otitis media, acute epiglottitis and meningitis. It may be present in nasopharynx or healthy adults and transmitted to vulnerable persons via respiratory droplet or contact of contaminated surfaces. 90% of invasive Hib disease affect children under the age of 5 years. Getting vaccinated is an effective way to prevent Hib disease.
Hib vaccine is incorporated into national vaccination scheme in various countries/ regions. To date, it is however not yet included in “Hong Kong Childhood Immunization Programme” by Department of Health. Hib vaccine is included in 5-in-1 or 6-in-1 combined vaccines. It is also available as standalone vaccine. Children can get vaccinated in private clinics.








